Endoscopic Spine Surgery
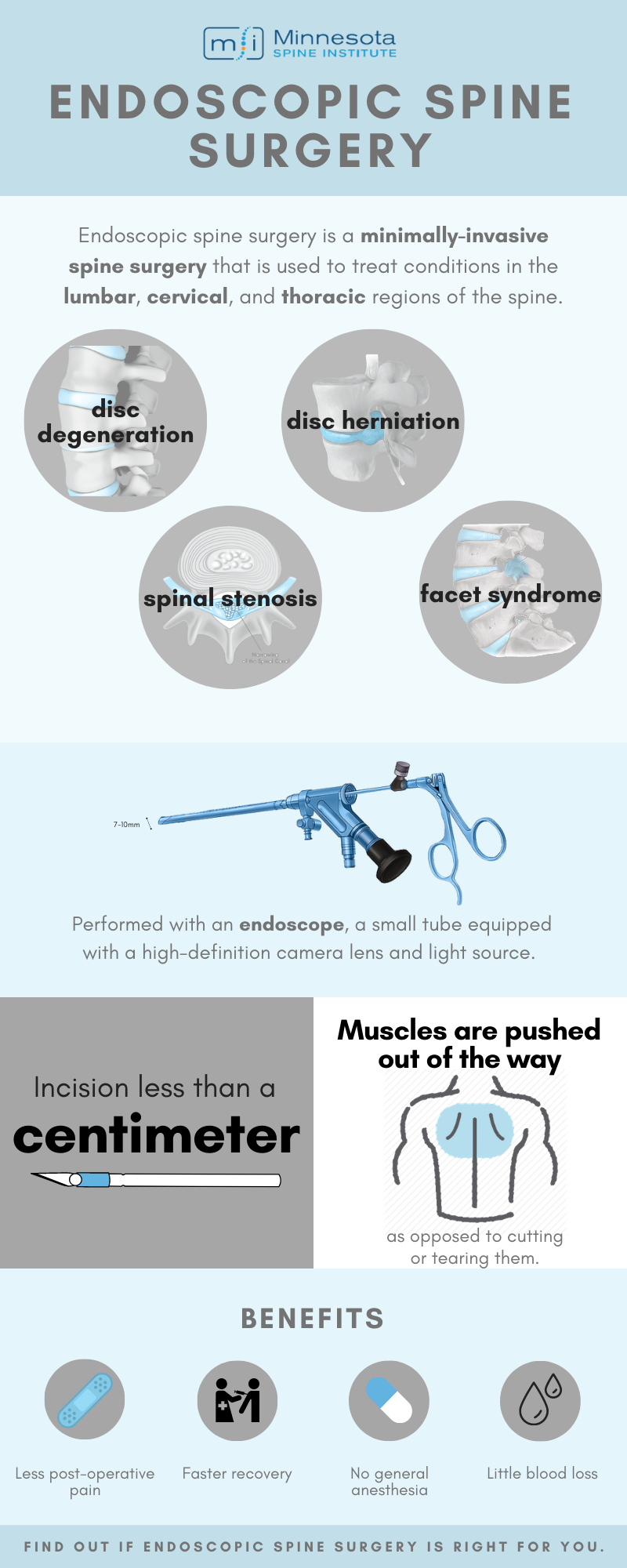
Endoscopic spine surgery is the most minimally invasive spine surgery technique that can be used to treat conditions in the lumbar, cervical, and thoracic regions such as spinal stenosis, foraminal stenosis, disc degeneration, and disc herniations.
The procedure
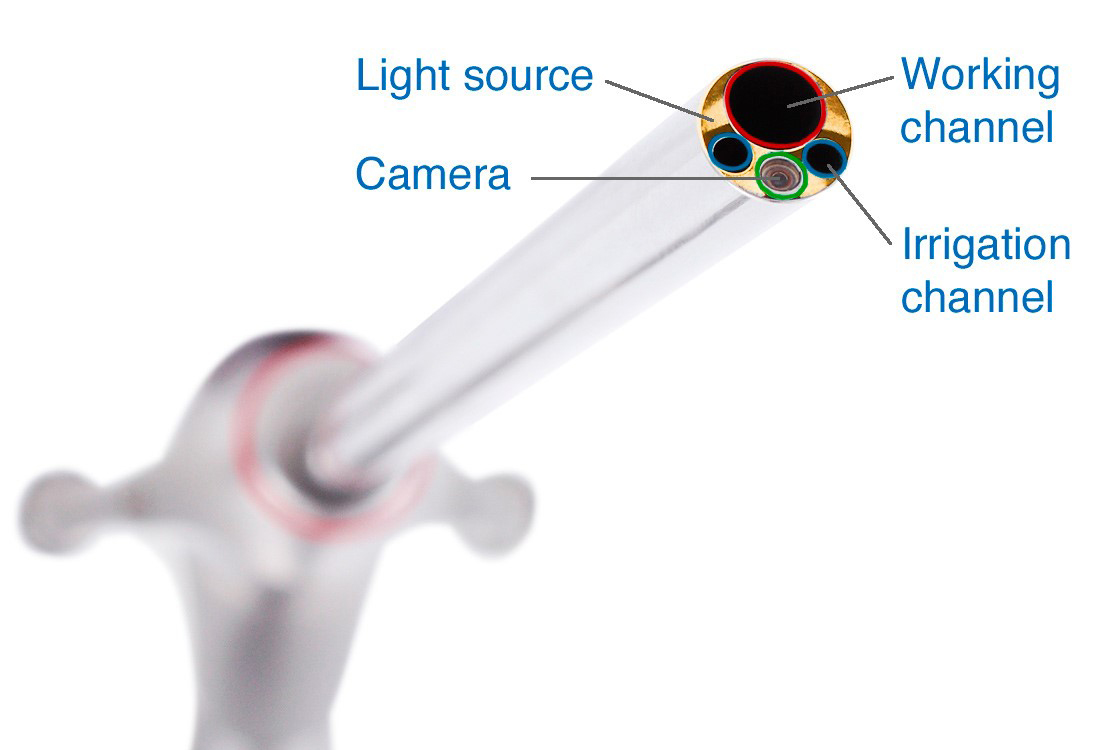
Endoscopic spine surgery is a type of minimally invasive surgery that is performed using an endoscope. An endoscope is a 7mm tube equipped with a high-resolution camera lens and a light source.
During the procedure, the surgeon makes an 8mm incision and gently divides the muscles to provide a small path for the endoscope to reach the spine. The endoscopic camera projects the images onto a monitor so the surgeon can visualize the anatomy & pathology. Small instruments are then inserted through the working channel to remove the problematic bone spurs, thickened ligament, or herniated disc material. When the procedure is complete, the surgeon removes the instruments and closes the incision with sutures.
The benefits of endoscopic spine surgery
Unlike traditional surgery, endoscopic techniques result in less damage to the surrounding spinal structures. During the procedure, the surgeon makes a skin incision, then gently divides the muscles, as opposed to cutting or tearing them, to create a small channel for the endoscope to fit through. This technique decreases muscle damage and therefore decreases weakness caused by traditional muscle retraction during open spine surgery.
Because endoscopic surgery is minimally invasive, general anesthesia is not always required, decreasing some medical risks and improving access to surgery for high-risk patients. Additionally, there is very little blood loss, a lower risk of infection, and the procedures are usually performed as same-day outpatient surgery. These benefits, along with the minimally invasive technique, result in less postoperative pain, a quicker recovery, and less need for postoperative narcotic pain medication. Our endoscopic patients normally do not require narcotic pain medication after endoscopic spine surgery.
Why isn’t all spine surgery done this way?
Not everyone can be treated with endoscopic spine surgery. Rarely, some conditions require a minimally invasive or traditional open approach. Although up to 90% of all spine surgeries are performed endoscopically in Asian and European countries, endoscopic spine surgery is a relatively new advancement in the treatment of spinal disorders in the United States.
These procedures require a unique combination of skills and training that take time to acquire. Dr. Hanson is the only surgeon in Minnesota who performs endoscopic hemilaminectomies, foraminotomies, microdiscectomies, and medial branch nerve transections. He has learned and perfected these skills through conferences around the United States and globally.
Find out if endoscopic spine surgery is an option for you. Schedule a consultation or contact us today.
